Diabetic Retinopathy
What is Diabetic Retinopathy?
Diabetic retinopathy is a complication of diabetes and a leading cause of blindness. It occurs when diabetes damages the tiny blood vessels nourishing the retina, the light-sensitive tissue inside the eye. This causes bleeding and swelling in the retina.
Who is at risk for Diabetic Retinopathy?
All people with diabetes - both type I and type 2 - are at risk. That is why everyone with diabetes should have a detailed eye exam at least once a year. More frequent eye checks are needed if you already have signs of retinopathy, poorly controlled diabetes, high blood pressure, or if you are pregnant.
What are the symptoms of Diabetic Retinopathy?
Symptoms include blurred vision, difficulty reading, floaters, and distorted vision. Early detection of diabetic retinopathy is essential for the preservation of vision. Don't wait for symptoms. Be sure to have a comprehensive dilated eye exam at least once a year.
My diabetes is under control, should I still have my eyes examined?
Some degree of diabetic retinopathy can occur despite good control of diabetes. All patients with diabetes should therefore have their eyes examined regularly. If you have diabetic retinopathy, at first you may notice no changes to your vision. But over time, diabetic retinopathy can get worse and cause vision loss.
How does Diabetic Retinopathy cause vision loss?
Retinal blood vessels damaged by diabetes can cause vision loss in several ways:
Fluid can leak into the macula, the part of the retina responsible for sharp detailed central vision. The fluid causes the macula to become swollen, hence blurring vision. This condition is called macular oedema.
Damaged blood vessels can become blocked with loss of blood flow to parts of the retina. This starves the retina of oxygen and nutrition. When it occurs in the macula, it causes central visual loss. This is called ischaemic maculopathy.
Fragile, abnormal blood vessels can grow in severe cases of retinopathy. These abnormal blood vessels can bleed into the jelly (vitreous) of the eye causing sudden loss of vision (vitreous haemorrhage). If left untreated, scar tissue can grow and pull on the surface of the retina to cause a retinal detachment. This advanced stage of the disease is called proliferative retinopathy and is potentially blinding.
-
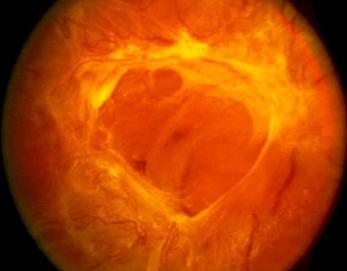
Proliferative diabetic retinopathy
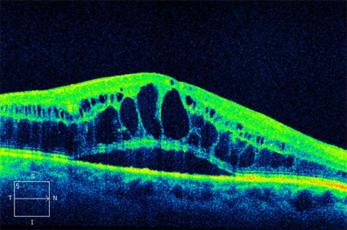
Diabetic macular oedema demonstrated on OCT
How is Diabetic Retinopathy treated?
During the early stages of diabetic retinopathy, no treatment is needed, but more frequent eye checks are usually needed. To prevent progression of diabetic retinopathy and vision loss, good control of blood sugar levels, blood pressure, and blood cholesterol are essential. Regular exercise and a sensible diet are also required. Your GP may enlist an endocrinologist to help with these points.
When there is more severe retinopathy or macular oedema, treatment with laser or injections into the eye is indicated. Sometimes surgery inside the eye is also needed in severe cases.
What happens during laser treatment?
Laser treatment is performed in the office of your eye specialist.
Before the treatment, your doctor will dilate your pupils and apply drops to numb the eye. The lights in the office will be dimmed. As you sit facing the laser machine, your doctor will hold a special contact lens to your eye. During the procedure, you will see flashes of light. The procedure usually takes about 10-15 minutes. Multiple laser sessions may be needed to complete the course of treatment.
After the treatment, you will need someone to drive you home because your vision will be a bit blur from the pupil dilation. You should also bring a pair of sunglasses to wear. There may be some discomfort after the laser and simple pain tablets (e.g. Paracetamol) can be taken for it.
Things to remember
- All patients with diabetes should have regular eye checks
- Good control of diabetes and regular eye examinations may prevent vision loss
- The earlier the retinopathy is detected and treated, the better the visual outcome
You will need the Adobe Reader to view and print these documents.
![]()







